Pearl is a clinical professor of plastic surgery at the Stanford University School of Medicine and is on the faculty of the Stanford Graduate School of Business. He is a former CEO of The Permanente Medical Group.
During my residency at Stanford, I traveled to Mexico with a group of surgeons to operate on children with cleft lips and palates. On the first day, I watched in awe as the team leader meticulously realigned the tissues of the lip, mouth and nose of a 3-month-old boy, leaving behind nothing but a faint scar — all in just 90 minutes.
I immediately fell in love with plastic and reconstructive surgery. As a surgeon, I visited over a dozen countries to repair the cleft lips and palates of children. But later, in my leadership role as CEO at Kaiser Permanente, extended travel proved impossible. And I missed those trips dearly.
Last month marked my first global surgery mission in many years. Not only did our time in the Philippines reignite my passion for global surgery, but it also left me with three surprising lessons for American health care:
Without mission and purpose, medicine proves exhausting
Surgical trips are physically and emotionally demanding. Far from the sterilized corridors of American hospitals, you are plunged into environments where resources are scarce and the needs overwhelming. In remote towns and underdeveloped cities, you operate in tight spaces with erratic electricity and limited clean water. The days stretch long, with five to seven surgeries in a 12-hour day.
Each child you treat carries a story of hardship and hope, their families’ eyes filled with a mix of fear and optimism. And just as you start to tire from the heat and yearn for a good night’s sleep, another mother arrives. She has walked for two days through the mountains with a child in her arms, praying her baby can be added to the surgical schedule. There is no saying “no” to this. You immediately become reinvigorated.
After a physically trying week, you return to the United States not exhausted, but emotionally replenished. Nearly every clinician who has participated in a surgical mission feels the exact same way.
American health care today obscures the fundamental mission and purpose that motivates clinicians. Physicians find themselves ensnared in a web of administrative tasks and insurance disputes. For many doctors, this noble calling has become just a job.
To revive the profession and address the burnout crisis that affects more than 60 percent of clinicians, a renaissance of purpose is imperative.
To get there, we must pivot away from the transactional “fee for service” financial model that rewards doctors for the sheer quantity of services rendered. In its place: a reimbursement model led by clinicians who are paid based on the quality of clinical outcomes achieved.
Inherent in the privilege of healing is the duty to lead this transformation. Taking on that accountability — and thereby eliminating the care restrictions that insurance companies impose — will rejuvenate, not further fatigue, health care professionals.
American doctors are excellent but so are physicians around the globe
U.S. physicians believe that training outside the States is a second-rate education. It’s time to alter that perspective.
During my week in the Philippines, I had the pleasure to work alongside five local physicians, often at adjoining operating room tables. They’d trained in residency and fellowship programs all around the world to maximize their expertise. To a person, their results matched the leading pediatric hospitals in the United States.
Although American doctors have access to the best facilities, machines and materials, physicians in other nations have a competitive advantage that comes from higher volume. The best way to hone any medical skill is through repetition and experience. American surgeons lag their global colleagues in this area.
U.S. clinicians bring a wealth of knowledge that can greatly benefit doctors worldwide, yet there are equally rich lessons to learn from the experiences and practices of physicians abroad.
In the U.S. today, doctors adhere to minimum surgical volume standards. Patient outcomes would improve tremendously if, instead, our nation set benchmarks for superior performance. Combining high-volume surgical experience with our advanced technologies and top-notch facilities would produce superlative clinical outcomes.
But first, America’s health care professionals need to embrace humility and be open to learning from our global colleagues.
U.S. resources are vast but access is still scarce
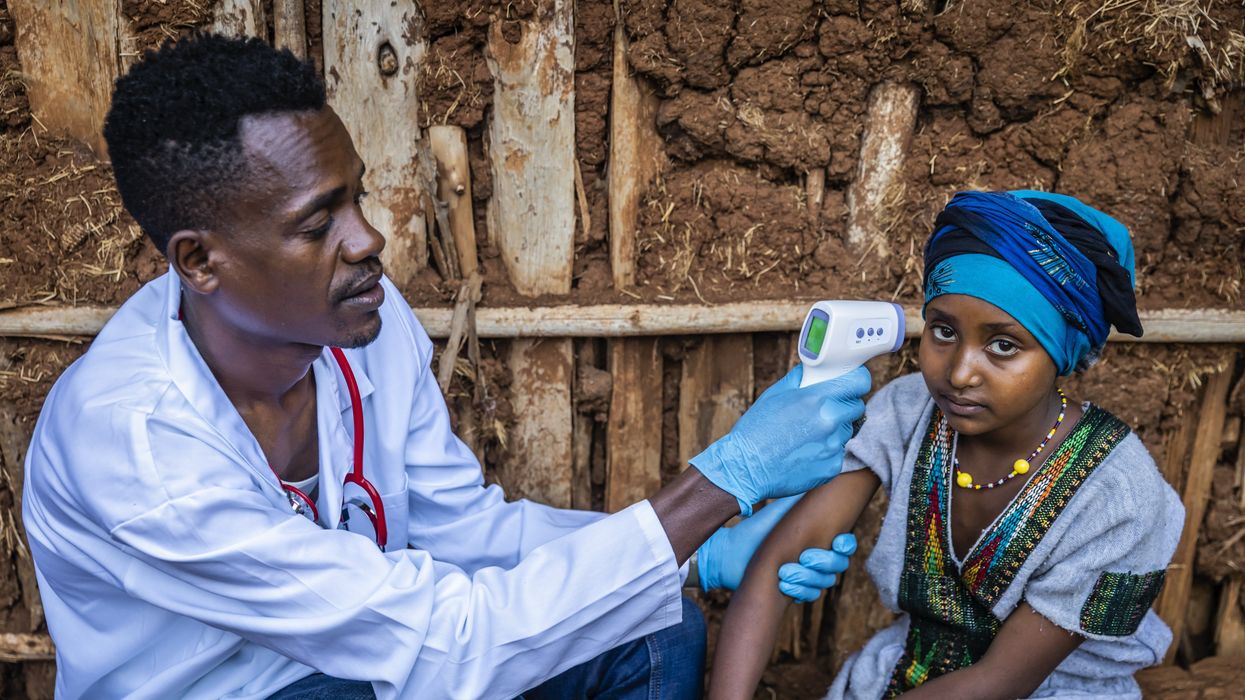
In countries like the Philippines, health care challenges are magnified by economic constraints. Despite government coverage, per capita health care spending remains low, under $200 annually. This financial reality forces difficult choices, leaving significant gaps between the health care needs of the population and the services available.
Witnessing these disparities firsthand is a poignant reminder of the abundance the United States enjoys, with health care spending now exceeding $13,000 per American. And yet, despite our nation’s wealth, independent studies reveal that U.S. health care ranks last among a dozen wealthy nations and near the bottom of 38 OECD countries in more than a dozen health measures.
The United States has earned its distinction as home to the most expensive and least effective health care system in the developed world. This isn’t just because of our 30 million uninsured citizens (and tens of millions who are underinsured). It’s the result of decades of underinvestment in primary care, tolerance of inefficient hospital systems and exorbitant drug prices.
The challenge of transforming American health care is daunting, and it requires a willingness to embrace change and confront uncomfortable truths. Observing the efficiency and ingenuity of less affluent nations inspires a reevaluation of our own care-delivery practices and health care finances.
The biggest problem in our health care system isn’t a lack of money. It’s the deficit in leadership and innovation.
Volunteering on global missions offers invaluable perspectives that could catalyze change in the United States. I’m optimistic that by learning from countries that achieve remarkable outcomes with modest means, we can enhance clinical outcomes, reduce clinician burnout, and make quality health care accessible and affordable for all Americans.